Incontinence
What is Incontinence?
Bladder incontinence is the involuntary loss of urine. Although the chance of becoming incontinent increases with pregnancy and/or age, it happens to people of all ages and is not a natural part of ageing.
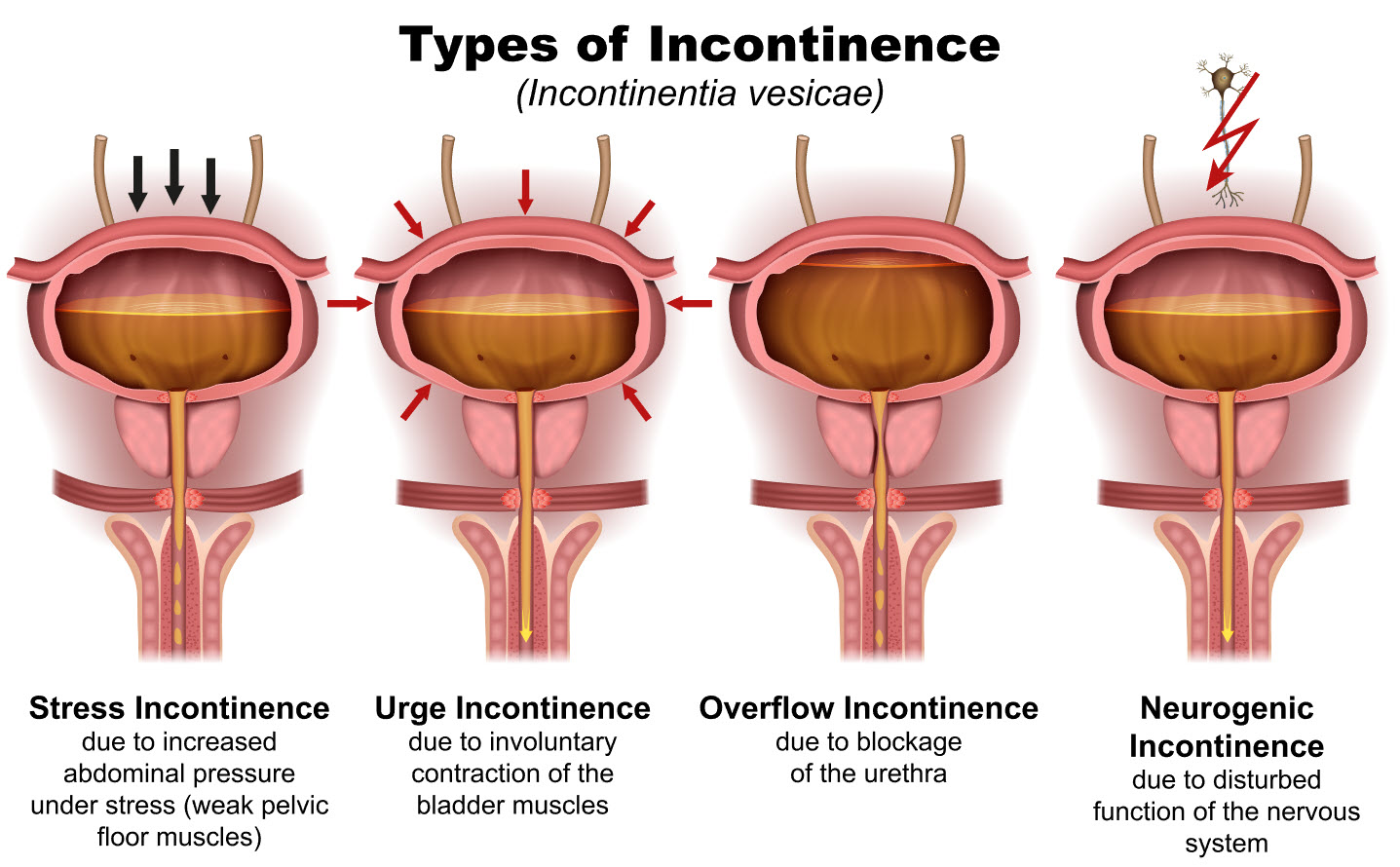
Classifications of Incontinence:
Stress – Loss of urine secondary to an increase in intra-abdominal pressure (coughing, sneezing, laughing, lifting, exercise or transitional movements)
Urge – Urine loss associated with a strong, uncontrollable need to void. Inability to delay voiding.
Mixed Incontinence – Urine loss associated with increases in intra-abdominal pressure (stress incontinence) AND with an intense urge to void (urge incontinence)
Functional – Urine loss associated with impairment of cognitive or physical function (eg. fractured hip), psychological unwillingness (dementia) or environmental barriers to the toilet
Overflow – Bladder does not empty normally and becomes very full (distended). Usually this is a neurological problem.
Benefits of Chartered Physiotherapy
Treatment for incontinence varies depending on what is causing it. We will perform an internal assessment of the muscles of your pelvic floor for both weakness and tension to determine the appropriate treatment plan to restore the function of your pelvic floor.
At Galway Physio Clinic, we use both internal palpation and real-time ultrasound ( http://galwayphysioclinic.ie/real-time-ultrasound-in-pelvic-health/ )to help you learn how to contract and strengthen your pelvic floor muscles. Research shows that up to 75% of women, based on verbal and written instruction alone, are not contracting their pelvic floor correctly. We will also help you learn behavioural changes involving diet and toileting patterns to decrease any irritations to the bladder/bowel.
Pelvic Organ Prolapse
What is Pelvic Organ Prolapse?
Pelvic Organ Prolapse is a subjective disorder described as an annoying protrusion at or near the vaginal opening, which may or may not be accompanied by perineal pressure or heaviness that may be aggravated by standing and relieved by lying down.
Types:
- Urethrocele – Prolapse of the urethra through the vagina
- Cystocele – Prolapse of bladder through the vagina
- Uterine Prolapse – Prolapse of uterus through the vagina
- Rectocele – Prolapse of rectus through the vagina
- Enterocele – Prolapse of the small intestine into the lower pelvic cavity. When this occurs, the small intestine pushes on the top part of the vagina, creating a bulge.
- Vault Prolapse – Occurs when the upper portion of the vagina loses its normal shape and sags or drops down into the vagina canal or outside the vagina. It may occur alone or along with any of the above examples of prolapse. This is a common complication following vaginal hysterectomy.
Benefits of Chartered Physiotherapy
Your pelvic floor muscles are the basket of muscles that support your organs against gravity and intra-abdominal pressure and your vaginal/rectal walls. These muscles may become weak as a result of childbirth or damage to part of the pelvic floor. As the pelvic floor becomes weak then it is no longer able to support your pelvic organs and these organs may then prolapse into the vagina. As well, the remaining muscles may become overloaded due to compensation and may develop some negative tension. We will assess the muscles of your pelvic floor for both weakness and tension to determine the appropriate treatment plan to restore the function of your pelvic floor.
Correctly performing specific pelvic floor strengthening exercises can help relieve the symptoms of the prolapse and result in a higher resting position of your bladder and bowel. Research shows that based on verbal and written instruction, 75% of women are doing their pelvic floor exercises incorrectly. At Galway Physio Clinic, we use both palpation and real-time ultrasound ( http://galwayphysioclinic.ie/real-time-ultrasound-in-pelvic-health/ ) to assess your ability to contract your pelvic floor muscles and teach you how to correctly strengthen your pelvic floor.
Diastasis Rectus Abdominis
What is Diastasis Rectus Abdominis?
Diastasis Rectus Abdominis is defined as a separation of the abdominal muscles which often can occur due to pregnancy or after prolonged abdominal loading with poor technique. The connective tissue where the abdominal muscles join in the midline is called the “linea alba”. The more this connective tissue is stretched sideways, the thinner and weaker it becomes. You may notice a bulge down the centre of your abdominals or that you can sink your fingers into the space in the midline of your tummy.
Benefits of Chartered Physiotherapy
At Galway Physio Clinic, we will do a comprehensive functional and real-time ultrasound examination ( http://galwayphysioclinic.ie/real-time-ultrasound-in-pelvic-health/ ) to determine the best treatment plan for restoring the function of your stretched abdominal wall and regain stability of your low back and pelvis. We will accurately measure the Inter-Recti Distance (IRD) with real-time ultrasound (this is the only way to accurately measure the separation) and monitor the IRD throughout your treatment program.
We aim to restore balance in your core muscles and re-educate the stretched connective tissue (linea alba) to facilitate tension across the abdominal wall. Exercises with optimal muscle recruitment are essential to restore the form and function of your abdominal wall. We use real-time ultrasound to help you visualise your diastasis rectus and muscle recruitment in order to facilitate your rehab.
When your abdominal muscles are stretched and separated, they are no longer able to adequately stabilise your low back and pelvis. Over time a diastasis can lead to other problems including lower back pain, pelvic instability, urinary incontinence/pelvic floor dysfunction, constipation and an increased risk of developing a hernia.
Real-time ultrasound in pelvic health
What is Real-Time Ultrasound in Pelvic Health?
Real-Time Ultrasound (RTUS) allows your Chartered Physiotherapist to gain a more accurate assessment of your abdominal and pelvic floor muscles at rest and during a contraction. We can watch the different layers of muscles contract, relax and most importantly look at their coordination, timing and size. It also provides real-time feedback for the patient who can visualise the muscles working on the screen, allowing them to learn and facilitate an improved pattern of muscle activation.
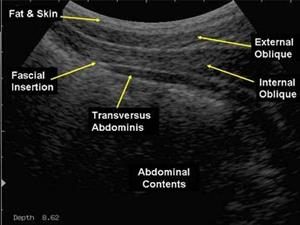
Benefits of Real-Time Ultrasound in Pelvic Health
The information gathered by the real-time ultrasound can be used for functional retraining for a variety of conditions such as diastasis recti, incontinence, pelvic organ prolapse, core strengthening and low back pain. The main muscles observed during the ultrasound are TVA, Internal oblique, External oblique, Rectus abdominus and the pelvic floor. Current research suggests that if you have low back or pelvic girdle pain or dysfunction (incontinence, vaginal, perineal or anal pain) or have been pregnant, these muscles may stop working effectively. These muscles are very important for stabilising your back, maintaining bladder and bowel control, and supporting your pelvic organs (bladder, uterus and rectum). As these muscles work effectively at a low amount of contraction, it can be difficult for people to learn the correct technique. The ultrasound gives you a picture of the muscle at rest and contracting, so you can see when you are contracting correctly. Real-time ultrasound is recognised as being safe as a therapeutic modality.
Postnatal Assessment
Seeing a Pelvic Health Physiotherapist in the postpartum period whether is it six weeks or six years later is essential for the rehabilitation and preventative care of the pelvic floor. Having carried and birthed a baby either vaginally or by caesarean are risk factors to developing pelvic floor dysfunction so we encourage every person during this life phase to see a Pelvic Health Physiotherapist.
Symptoms can present later in life so starting early will help set you on the right track. Postnatally, pelvic floor physiotherapists will assess:
- Pelvic floor muscles (strength/length)
- Integrity of C-section scar, episiotomy scar or vaginal tears
- Diastasis rectus abdominus (separation of the rectus abdominus musculature)
- Any physical problems arising from pregnancy and childbirth
- Your thoughts/beliefs/attitudes and how it affects your physical well-being
- Readiness to return to activities and/or sport
The most common dysfunctions that may occur in the postpartum period include pelvic pain, sexual pain and incontinence (bladder or bowel). There are numerous reasons for postpartum pain and incontinence; however, some common explanations include: weakened muscles, scar tissue development from episiotomies or tears, prolapse and hormonal changes. Treatment includes hands-on therapy, pelvic floor and abdominal home exercise programming, and lifestyle recommendations to prevent recurrence.
Contrary to popular belief, you do not need to live with incontinence, pelvic pain as a side effect of motherhood. If you are experiencing bladder control issues or pelvic floor pain when you sneeze, cough, or in the middle of your fitness routine, we can help.

Return to Running/High Impact Activity
You have had your baby and have been given clearance from your medical team to begin exercise. You would like to get back into shape, but how do you transition to exercise safely? What acitivites are safe to perform postnatally? When is a good time to start high impact activites like running or circuit/HITT training? Are you experiencing pain or intcontinece with running or other hight impact activities?
Our Pelvic health physiotherapist will ask what your concerns are regarding returning to running or hight impact activities. Assess the strength, function and coordination of you pelvic floor and abdominal musculature. Assess the ability of your pelvic floor, abdominals, low back and pelvis reacts and absorbs impact. We will then put together a custom plan to help improve your levels of activity and quality of life.


